That sharp, throbbing pain in just one spot on your gums can be both puzzling and uncomfortable. If you’re dealing with localized gum discomfort that won’t go away, you’re not alone – this targeted pain affects millions of people and usually signals something specific happening in that exact area.
This guide is for anyone experiencing gum pain in a single location who wants to understand what’s causing it and how to find relief. We’ll explore the most common causes of localized gum pain, from minor irritation to more serious dental conditions that need professional attention. You’ll also discover quick relief methods you can try at home and learn when it’s time to see your dentist for proper treatment.
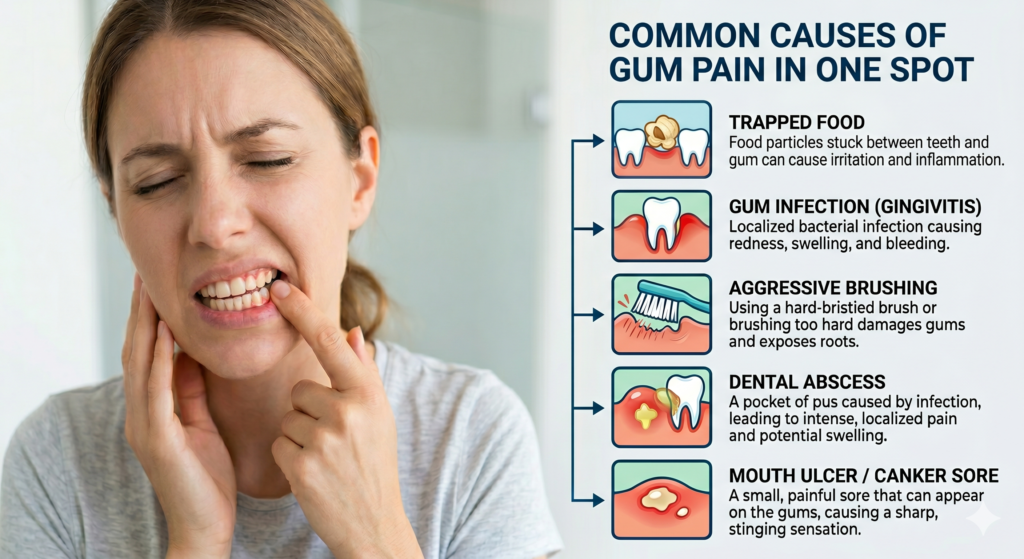
Common Causes of Localized Gum Pain
Gingivitis and Early Gum Disease
Gingivitis ranks as the most common culprit behind localized gum pain. This mild form of gum disease develops when bacteria accumulate along the gum line, creating a sticky film called plaque. The bacteria release toxins that irritate your gums, causing inflammation, tenderness, and often bleeding during brushing or flossing.
What makes gingivitis particularly sneaky is how it can affect just one area of your mouth. Poor oral hygiene in specific spots, like hard-to-reach molars or areas around dental work, creates perfect conditions for bacterial buildup. You might notice your gums appear redder than usual or feel swollen in the affected area.
The good news? Gingivitis responds well to improved oral care. Regular brushing, flossing, and professional cleanings can reverse the condition before it progresses to more serious periodontal disease.
One of the main reasons for this is plaque buildup along the gum line. If you want to remove it effectively, check out our detailed guide on how to remove plaque from teeth naturally at home.
Food Particles Trapped Between Teeth
Small pieces of food wedged between your teeth and gums can cause surprising discomfort. Foods like popcorn kernels, sesame seeds, or fibrous vegetables often get stuck in tight spaces, pressing against gum tissue and creating irritation.
This trapped debris acts like a splinter, causing localized pain that can range from mild annoyance to sharp discomfort. The longer food particles remain lodged, the more inflammation develops as bacteria feed on the debris and multiply.
Common problem foods include:
- Popcorn hulls and kernels
- Seeds from berries or bread
- Stringy meats
- Raw vegetables like celery or corn
Aggressive Brushing or Flossing Technique
Enthusiastic oral care can backfire when you brush or floss too vigorously. Aggressive brushing with a hard-bristled toothbrush can damage delicate gum tissue, creating small wounds that become painful and inflamed.
Many people make the mistake of thinking harder brushing means cleaner teeth, but this approach often leads to gum recession and sensitivity. Similarly, forceful flossing can cut into gums, especially if you’re just starting a flossing routine or using improper technique.
Signs of aggressive oral care include:
- Bleeding after brushing or flossing
- Gums that feel raw or tender
- Recession along the gum line
- Worn toothbrush bristles after short use
Using an old or hard toothbrush can worsen gum damage. Make sure you’re using the right one by reading how often you should replace your toothbrush.
Canker Sores and Mouth Ulcers
Canker sores can develop on gum tissue, creating intense localized pain that makes eating, drinking, and even talking uncomfortable. These small, shallow ulcers appear as white or yellow centers surrounded by red, inflamed tissue.
Unlike cold sores caused by viruses, canker sores aren’t contagious but can be triggered by minor injuries, stress, certain foods, or immune system fluctuations. When they appear on gums, they often result from accidental bites, dental work irritation, or sharp edges on teeth or dental appliances.
The pain from canker sores typically peaks within the first few days and gradually subsides over 7-14 days as the ulcer heals naturally.
Dental Issues That Trigger Single-Spot Gum Pain
Tooth Decay Near the Gum Line
Cavities don’t always announce themselves with obvious pain in the tooth itself. When decay develops close to where your tooth meets your gum, it creates a perfect storm for localized gum irritation. The bacteria that cause cavities produce acids that eat away at tooth enamel, and when this happens near the gum line, your gums become collateral damage.
Your gums respond to this bacterial invasion by becoming inflamed, swollen, and tender in that exact spot. You might notice the pain gets worse when you bite down or touch the area with your tongue. The tricky part is that early-stage decay near the gum line often goes unnoticed during regular brushing because the cavity sits in a hard-to-reach spot.
Food particles and plaque love to hide in these areas, feeding the bacteria and making the problem worse. If you’re experiencing persistent gum pain in one location, especially if it’s accompanied by sensitivity to hot or cold foods, decay near the gum line could be the culprit.
Cracked or Damaged Teeth
A crack in your tooth might seem like it would only affect the tooth itself, but damaged teeth often create significant gum problems. When a tooth cracks, it creates an opening where bacteria can sneak in and set up camp. This bacterial invasion doesn’t stay confined to the tooth—it spreads to the surrounding gum tissue.
Vertical cracks that run from the chewing surface down toward the root are particularly problematic. These cracks can extend below the gum line, creating a direct pathway for bacteria to reach areas that are normally protected. Your gums react by becoming inflamed and painful right at the site of the crack.
Broken fillings or crowns can cause similar issues. When dental work fails, sharp edges or gaps develop that irritate your gums every time you chew or speak. The constant trauma keeps the gum tissue in a state of inflammation, leading to persistent pain in that specific area.
Even hairline fractures that you can’t see can cause gum pain. These micro-cracks allow bacteria to penetrate deeper into the tooth structure, and your gums respond with inflammation as your body tries to fight off the infection.
You may also notice bleeding while brushing, which is a common warning sign. Learn more about it in our article on why do my gums bleed when I brush.
Impacted Wisdom Teeth
Wisdom teeth have a reputation for causing trouble, and localized gum pain is often their calling card. When these third molars don’t have enough room to emerge properly, they become impacted, creating a host of problems for the surrounding gum tissue.
Partially erupted wisdom teeth are the biggest troublemakers. They create a flap of gum tissue that acts like a pocket where food and bacteria accumulate. This area becomes almost impossible to clean properly with regular brushing and flossing, leading to infection and inflammation in that specific spot.
The pressure from an impacted wisdom tooth trying to push through can cause the overlying gum tissue to become swollen and extremely tender. You might notice the pain gets worse when you open your mouth wide or chew on that side. Sometimes the pain radiates to your jaw or ear, but it typically starts as a sharp, localized discomfort right over the impacted tooth.
Infection around impacted wisdom teeth can develop quickly and become serious. The gum tissue may appear red and swollen, and you might taste something unpleasant when you bite down. Bad breath often accompanies these infections because bacteria multiply rapidly in the warm, moist environment created by the gum flap.
Serious Conditions Behind Targeted Gum Discomfort
Advanced Periodontal Disease
Gum pain that feels concentrated in one spot could signal advanced periodontal disease, where bacteria have established deep pockets between your teeth and gums. Unlike early-stage gingivitis that affects larger areas, advanced periodontitis often creates localized inflammation that feels like a persistent ache or sharp pain in specific spots.
When periodontitis progresses, it destroys the tissues and bone supporting your teeth. You might notice the affected area feels tender to touch, bleeds easily, or has a bad taste. The pain typically worsens when eating or brushing, and you may see your gums pulling away from teeth, creating visible gaps.
Advanced periodontal disease doesn’t just cause discomfort—it can lead to tooth loss if left untreated. The infection can also spread to other parts of your mouth or even enter your bloodstream, potentially affecting your overall health.
Gum Abscesses and Infections
A gum abscess creates intense, throbbing pain that’s impossible to ignore. This bacterial infection forms when harmful bacteria get trapped in your gum tissue, creating a pocket of pus that causes severe localized pain. The affected area often swells significantly and feels warm to the touch.
Unlike general gum soreness, an abscess produces sharp, radiating pain that can extend to your jaw, ear, or neck. You might experience facial swelling, fever, and a foul taste in your mouth. The pain often intensifies when you lie down, making sleep difficult.
Dental abscesses require immediate professional treatment because the infection can spread rapidly. Without proper care, the bacteria can enter your bloodstream or affect nearby tissues, creating serious health complications. Some people try to manage the pain with over-the-counter medications, but this only masks the symptoms while the underlying infection continues to worsen.
Oral Cancer Warning Signs
Persistent gum pain in one location sometimes indicates oral cancer, especially when accompanied by other concerning symptoms. Early-stage oral cancer can appear as a small, painless sore that gradually becomes more uncomfortable over time.
Watch for these warning signs alongside localized gum pain:
- Sores that don’t heal after two weeks
- White or red patches on your gums
- Unusual lumps or thickened areas
- Persistent bleeding without obvious cause
- Numbness in your mouth or lips
- Changes in how your teeth fit together
Oral cancer pain often starts as mild discomfort but gradually intensifies. The affected area might feel different when you run your tongue over it – perhaps rougher or more sensitive than surrounding tissue. Some people describe a burning sensation or persistent soreness that doesn’t respond to typical oral care measures.
Early detection significantly improves treatment outcomes for oral cancer. Regular dental checkups help catch potential problems before they become serious, which is why persistent gum pain should never be ignored.
Autoimmune Disorders Affecting Gums
Several autoimmune conditions can cause targeted gum pain by making your immune system attack healthy gum tissue. Lichen planus, lupus, and pemphigoid commonly affect oral tissues, creating painful lesions that feel like burning, stinging, or aching in specific spots.
These conditions often produce distinctive symptoms that differ from typical gum problems. You might notice white, lacy patterns on your gums, painful blisters that break easily, or areas of tissue that appear red and inflamed. The pain can be constant or come in waves, and certain foods or beverages might trigger increased discomfort.
Autoimmune-related gum pain typically doesn’t respond well to standard oral hygiene improvements. The affected areas might look different from healthy gum tissue – sometimes appearing shiny, scarred, or discolored. Many people with these conditions also experience similar symptoms in other parts of their body, helping doctors recognize the underlying autoimmune connection.
Managing autoimmune disorders requires specialized treatment that addresses the root cause rather than just the symptoms. Your dentist and physician often work together to develop an effective treatment plan that reduces inflammation and protects your oral health.
Quick Relief Methods for Immediate Comfort
Salt Water Rinses for Natural Healing
Warm salt water rinses work like magic for soothing inflamed gums. Mix half a teaspoon of salt into a cup of warm water and swish gently around the affected area for 30 seconds. The salt draws out bacteria and reduces swelling while promoting faster healing. Do this three to four times daily, especially after meals and before bed.
The beauty of salt water lies in its simplicity and effectiveness. Salt creates an environment where harmful bacteria can’t thrive, while the warm temperature increases blood flow to the area. This combination helps your body’s natural healing process kick into high gear. Make sure the water isn’t too hot – you want it comfortably warm, not scalding.
For best results, don’t eat or drink anything for at least 30 minutes after rinsing. This gives the salt time to work its antimicrobial magic. You’ll often notice reduced pain and swelling within the first day of consistent use.
Cold Compress Application Techniques
Cold therapy works wonders for numbing pain and reducing inflammation in your gums. Wrap ice cubes in a thin towel or use a cold pack, then apply it to the outside of your cheek near the painful spot for 15-20 minutes at a time.
Never apply ice directly to your skin – always use a barrier like a towel or cloth. Take breaks between applications to prevent tissue damage. You can repeat this process every few hours throughout the day as needed.
| Application Method | Duration | Frequency |
|---|---|---|
| Ice pack with towel | 15-20 minutes | Every 2-3 hours |
| Cold wet cloth | 10-15 minutes | Every hour |
| Frozen peas in towel | 15 minutes | Every 2 hours |
Cold compresses work best in the first 48 hours after pain begins. The cold temperature constricts blood vessels, reducing inflammation and providing temporary pain relief. Some people find alternating between cold and warm compresses helpful, but start with cold if swelling is present.
Over-the-Counter Pain Management Options
Several effective pain relievers can help manage gum pain while you address the underlying cause. Ibuprofen stands out as the top choice because it tackles both pain and inflammation. Take 400-600mg every six to eight hours with food to prevent stomach upset.
Acetaminophen offers another solid option, especially if you can’t take NSAIDs due to stomach issues or blood thinners. Follow the package directions carefully – typically 500-1000mg every four to six hours, not exceeding 4000mg in 24 hours.
Topical gels containing benzocaine or lidocaine provide direct numbing relief when applied to the affected gum tissue. These work quickly but only last for short periods. Popular brands include Orajel and Anbesol. Apply a small amount directly to the painful area using a clean finger or cotton swab.
Oral rinses with antiseptic properties can also help. Look for mouthwashes containing cetylpyridinium chloride or hydrogen peroxide. These kill bacteria while providing mild pain relief. Avoid alcohol-based rinses as they can irritate already sensitive gums.
Remember that over-the-counter solutions provide temporary relief while your body heals or until you can see a dentist for persistent problems.
Professional Treatment Options for Persistent Pain
Deep Cleaning and Scaling Procedures
When gum pain persists in one spot, your dentist might recommend deep cleaning procedures that go beyond regular dental cleanings. Root planing and scaling target the infected areas below the gum line where bacteria love to hide. During scaling, your dental hygienist uses specialized tools to remove hardened plaque and tartar buildup from tooth surfaces and beneath the gums. Root planing smooths out rough spots on tooth roots where bacteria tend to gather.
These procedures typically require local anesthesia since they involve cleaning deeper pockets around your teeth. You might experience some sensitivity and mild discomfort for a few days afterward, but this usually signals that your gums are beginning to heal. Many patients notice significant improvement in localized pain within a week or two as inflammation decreases.
The process might be split across multiple appointments, especially if several areas need attention. Your dentist will monitor healing progress and may schedule follow-up visits to ensure the infection clears completely.
Antibiotic Therapy for Infections
Bacterial infections causing localized gum pain often require antibiotic treatment alongside professional cleaning. Your dentist might prescribe oral antibiotics like amoxicillin or doxycycline to fight the specific bacteria causing your symptoms. These medications work from the inside out, reaching areas that topical treatments can’t access effectively.
Antibiotic mouth rinses provide another treatment option, delivering medication directly to the affected area. Chlorhexidine rinses are particularly effective against the bacteria that cause gum disease and can reduce inflammation in targeted spots.
Some dental offices use antibiotic gels or fibers placed directly into infected gum pockets. These localized treatments deliver high concentrations of medication exactly where it’s needed while minimizing side effects on the rest of your body. Treatment duration varies depending on infection severity, but most patients see improvement within several days of starting antibiotic therapy.
Surgical Interventions for Severe Cases
Persistent gum pain that doesn’t respond to conservative treatments might require surgical intervention. Flap surgery allows your periodontist to lift back gum tissue, providing direct access to clean infected roots and remove diseased tissue. This procedure helps eliminate deep bacteria pockets that cause ongoing pain and inflammation.
Gum grafts address cases where gum recession exposes tooth roots, causing sensitivity and discomfort in specific areas. During this procedure, tissue from another part of your mouth covers the exposed root surface, reducing pain and preventing further recession.
Bone grafting becomes necessary when infection has damaged the bone supporting your teeth. Your surgeon places bone graft material in the affected area to encourage new bone growth and restore stability to loose teeth causing pain.
Laser therapy offers a less invasive alternative for some patients. Dental lasers can remove infected tissue and bacteria while promoting healing in the treated area. This option typically involves less discomfort and faster recovery times compared to traditional surgery.
Restorative Dental Work Solutions
Sometimes localized gum pain stems from dental work that needs repair or replacement. Poorly fitting crowns or fillings can irritate gums and create pockets where bacteria accumulate. Your dentist might need to adjust or remake these restorations to eliminate the source of irritation.
Crown lengthening procedures can help when there isn’t enough tooth structure above the gum line to properly support a restoration. This surgery reshapes gum tissue and sometimes bone to expose more of the natural tooth, allowing for better-fitting crowns or fillings.
Dental implants might be recommended if a damaged tooth is causing ongoing gum problems. Removing the problematic tooth and replacing it with an implant can eliminate the source of infection and pain while restoring full function to the area.
Root canal therapy addresses cases where tooth infection spreads to surrounding gum tissue. This procedure removes infected pulp from inside the tooth, often resolving both tooth and gum pain in the affected area.
Prevention Strategies to Avoid Future Gum Problems
Proper Daily Oral Hygiene Routine
Brushing twice daily with fluoride toothpaste forms the foundation of gum health. Use a soft-bristled toothbrush and gentle circular motions, spending at least two minutes cleaning all surfaces. Pay special attention to the gumline where plaque accumulates most. Replace your toothbrush every three months or sooner if bristles become frayed.
Flossing daily removes food particles and bacteria from between teeth where your toothbrush can’t reach. If traditional floss feels difficult, try water flossers, floss picks, or interdental brushes. The key is finding a method you’ll actually use consistently.
Consider adding an antimicrobial mouthwash to your routine, especially one designed for gum health. Rinse for 30 seconds after brushing and flossing to help reduce bacteria levels in your mouth.
Don’t forget your tongue – bacteria can harbor there and contribute to gum problems. Use a tongue scraper or gently brush your tongue during your regular routine.
Regular Dental Checkups and Cleanings
Professional cleanings every six months remove tartar buildup that home care can’t address. During these visits, your dental hygienist can spot early signs of gum disease and provide personalized advice for your specific needs.
Your dentist can identify problem areas before they become painful and expensive to treat. They’ll measure pocket depths around your gums and check for signs of inflammation or infection that might not be obvious to you.
If you have a history of gum problems, your dentist might recommend more frequent cleanings – every three to four months instead of twice yearly. This proactive approach can prevent minor issues from developing into serious conditions requiring extensive treatment.
Dietary Changes for Healthier Gums
What you eat directly impacts your gum health. Limit sugary and starchy foods that feed harmful bacteria in your mouth. When you do indulge, rinse with water afterward to help wash away residue.
Incorporate foods rich in vitamin C, like citrus fruits, berries, and leafy greens, which support gum tissue health and healing. Vitamin D from sources like fatty fish and fortified foods helps your body absorb calcium and supports immune function.
Crunchy fruits and vegetables like apples, carrots, and celery naturally help clean teeth and stimulate saliva production. Saliva neutralizes acids and helps wash away food particles throughout the day.
Stay hydrated by drinking plenty of water, which helps maintain healthy saliva levels and rinses away bacteria. Avoid excessive alcohol consumption, which can dry out your mouth and increase infection risk.
Consider foods with natural anti-inflammatory properties, such as green tea, which contains compounds that may help reduce gum inflammation when consumed regularly.
Conclusion
When your gums hurt in just one spot, it’s usually your mouth’s way of telling you something needs attention. From simple irritation caused by aggressive brushing to more serious issues like gum disease or dental abscesses, localized gum pain often has a clear cause that can be addressed. The key is recognizing when the discomfort signals something that needs professional care versus something you can handle at home with gentle cleaning and over-the-counter pain relief.
Don’t ignore persistent gum pain that lasts more than a few days or gets worse over time. Your dentist can quickly identify what’s causing the problem and recommend the right treatment to get you back to comfort. Meanwhile, stick to gentle oral care habits, avoid irritating the area, and remember that good daily brushing and flossing are your best defense against future gum problems. Your gums do important work protecting your teeth, so giving them the care they deserve will pay off in the long run.
Frequently Asked Questions
Q1: Why do my gums hurt in one specific spot?
Localized gum pain is usually caused by food stuck between teeth, gum infection, or irritation from brushing too hard. It can also indicate early gum disease.
Q2: Is gum pain in one area serious?
Not always, but if the pain lasts more than a few days, worsens, or includes swelling or pus, it may indicate an infection and should be checked by a dentist.
Q3: Can food stuck in gums cause pain?
Yes, trapped food particles can irritate the gum tissue and lead to inflammation, causing sharp pain in one spot.
Q4: How can I relieve gum pain at home?
You can try salt water rinses, cold compress, and maintaining proper oral hygiene. Avoid aggressive brushing and irritating foods.
Q5: When should I see a dentist for gum pain?
Visit a dentist if:
- Pain lasts more than 3–5 days
- You notice swelling or pus
- There is bleeding or bad breath
- Pain becomes severe
Q6: Can stress cause gum pain in one spot?
Yes, stress can lead to teeth grinding (bruxism), which may cause pressure and irritation in specific gum areas.
Author
Monali Singh is a health content researcher who writes about wellness, dental care, and nutrition. She focuses on simplifying complex health topics for everyday readers.
